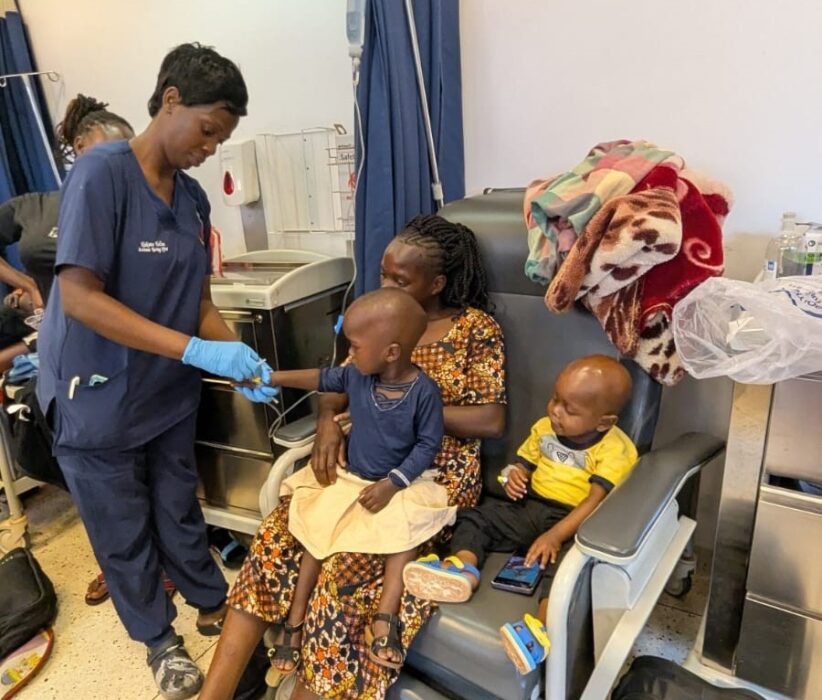
Amanda Semerene is a Research Nurse in the Paediatric Oncology Department at Cambridge University Hospitals NHS Foundation Trust (CUH). Following a recent visit to Kampala, here she explains the value of being able to work face-to-face with fellow nurses at the Uganda Cancer Institute.
“The Paediatric Cancer Health Partnership is a partnership between staff at Cambridge University Hospitals NHS Foundation Trust (CUH) and staff at the Uganda Cancer Institute. Supported by CGHP, it aims to improve care for children with cancer, for example by speeding up diagnosis and ensuring the safe and effective administration of chemotherapy.
After many months of remote working, the primary aim of this visit was to assess and embed a Paediatric Oncology triage tool into the Outpatient Department (OPD). The tool had already been audited at CUH in the months leading up to the visit, with remote support from the Ugandan team. Its purpose is to identify the unwell child at the point of arrival/ assessment in the OPD.
The secondary aim was to improve links between UCI and CUH nursing staff to collaborate on future projects. The visit focused on understanding the layout of the paediatric oncology service and the provisions and the process – in particular of chemotherapy – through the department.
The visit was unique in comparison to previous trips undertaken by the CUH team to UCI as it was particularly focused on establishing nursing relationships, rather than on medical partnerships.


Building knowledge in-person
I started by getting a feel for the layout of the ward and the OPD, having conversations with the nursing team and building a better understanding of the level of care required for their inpatients.
We started testing the triage too on day two, which was an opportunity to see the flow of patients through the OPD and to observe how it would fit with the pressures of the department. We were also able to review the completed triage tool used during the audit, which showed us which areas had been used and what the essential information was.
Having seen the pressures of the department, with high volumes of patients and low numbers of staff, it was challenging to see how the triage tool could be implemented with good effect. However, when we talked to those who’d used it during the audit, we could see the value that it had added to their systems. The UCI nurses commented that the tool had given them confidence to highlight patients they were concerned about to the medical team. It had also provided them and the patients’ families with education.
We worked together as a team to collate the feedback and refine the tool so that it included all necessary information to identify the unwell child. We were able to make practical changes to make it more suitable for the UCI environment – for example making it smaller and making it printable so that it didn’t add additional paper to the medical notes. Over the course of the week we continued to improve the triage tool to make it a user friendly as possible and allowing the nursing team to review it. Day five was implementation day, where we presented the nursing team with printed resources and ways to store the triage tool pre and post use.
We also had chance to observe the flow of chemotherapy from prescription to infusion into the patients, giving us lots of insight for future projects.


The impact of working as team
I consider myself a team player and struggle to think about individual impact. But I think the biggest value that I offered was my quieter ability to observe and notice, and my confidence to be able to keep us to task. I was integral in collating all the data from the previously undertaken audit, bringing ideas such as making small versions of the tool in colour and laminating as pocket guides for the nursing team. I was also able to pioneer the idea of placing a simpler triage tool, focusing on the key prompts, onto the developing assessment slip. Working as a team really did enable collaborative ideas to create a stronger output in the end.
The most challenging time was when we didn’t think the tool was going to be able to be implemented, and after such a lot of remote working this was frustrating. But we also couldn’t move forward on something that wouldn’t help or be useable. Conversely the most rewarding part was finding out when we were home that the tool was being used and was a success.
I think one of the most impactful moments was the sheer determination of under-resourced, over-pressured nurses to continue to think outside the box, challenging what was possible so they could continue to grow and develop for the good of the children they treat.
Personal and professional growth
I spend most of my time personally and professionally working quietly and valuing the gains of my team, rather than personal gains. The visit has made me think more about the benefit of sharing my ideas, in order to share knowledge and experiences.
The visit has also challenged me to think about some of our ways of working within the NHS, and to consider what actually impacts and makes a difference to our patients. For example, the pressure on the staff in Uganda means there is a big responsibility on the parents to be involved in many of the processes of their child’s treatment. While this sometimes might be a huge burden on the parents, for example when they have to source and pay for their child’s chemotherapy, there are also areas where I think parents at CUH lose control over their child’s treatment that leaves them feeling powerless. I am keen to share my experiences with individuals in my department, and explore how we can offer parents more control over their child’s healthcare. A next step would be inviting some of the nursing team from UCI to visit CUH.
Looking ahead
Our expectation is that the tool will be used to identify the unwell or deteriorating child, through knowledge and empowerment of the nursing team, which will impact the long-term outcomes for this vulnerable group of patients.
I also have small scale and larger scale ideas of how we could develop our nursing relationship with UCI. For example, standard operating procedures (SOPs) for spillage, or audits of UCI nursing/medical and parental tasks in comparison with CUH and reviewing the impact this might have on long term outcomes. It would also be interesting to consider how the learnings from UCI could be relatable in other settings.

Final reflections
Having worked in the NHS all my career, experiencing something different is always good. Global health has always been of interest to me, particularly with Paediatric Oncology services, and working with GCHP has given me a legitimacy to explore this further. Being given the opportunity to understand healthcare systems through practical experience rather than theory is revolutionary. I have come back challenged with the idea of how the care we offer can meet more in the middle between UCI and CUH.”
Find out more about the Paediatric Cancer Health Partnership.
Return to blogs

