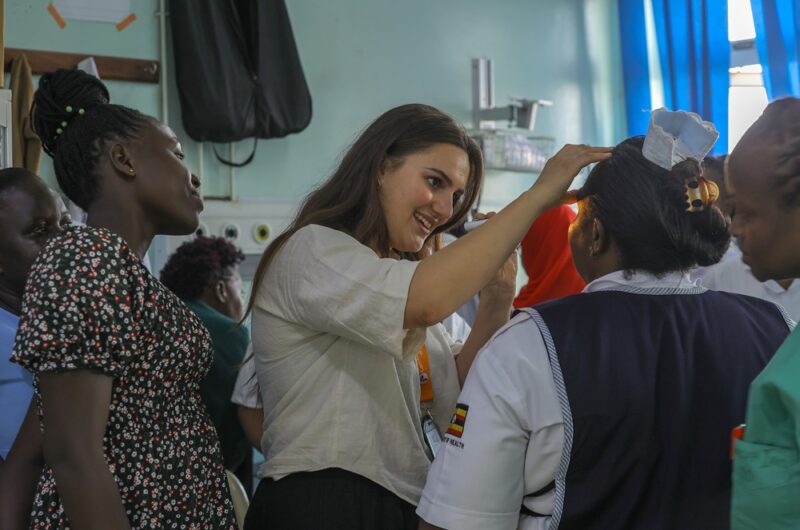By Madeleine Custerson
Madeleine Custerson is a Staff Nurse in the Neurosciences Critical Care Unit (NCCU) at Addenbrooke’s Hospital. Here she describes the enormous impact of a week learning and teaching alongside nurses in Uganda as part of the SCALE Critical Care Project.
“I have always had a keen interest in global health and chose to get involved in this project to grow both personally and professionally. I felt disconnected from nursing in the UK and was seeking fresh perspectives, cultural exposure, and new challenges. The opportunity to step outside my routine and experience healthcare in a different country reignited my passion and reminded me of the wide-reaching opportunities this profession can offer.
Now, having experienced global health firsthand, I have a much deeper understanding of its impact and significance. It highlighted to me the values that brought me into nursing in the first place: compassion, kindness and making a difference to people’s lives.
The SCALE Critical Care Project has the overall aim of strengthening critical care capacity and capability in Uganda and the UK. It facilitates a collaborative learning environment and ensures sustainability to improve clinical practice and patient outcomes. I hope that our trip and all future trips will lead to lasting improvements in skills in both Ugandan and UK healthcare professionals, systems and patient care.


Teaching and learning in Kampala
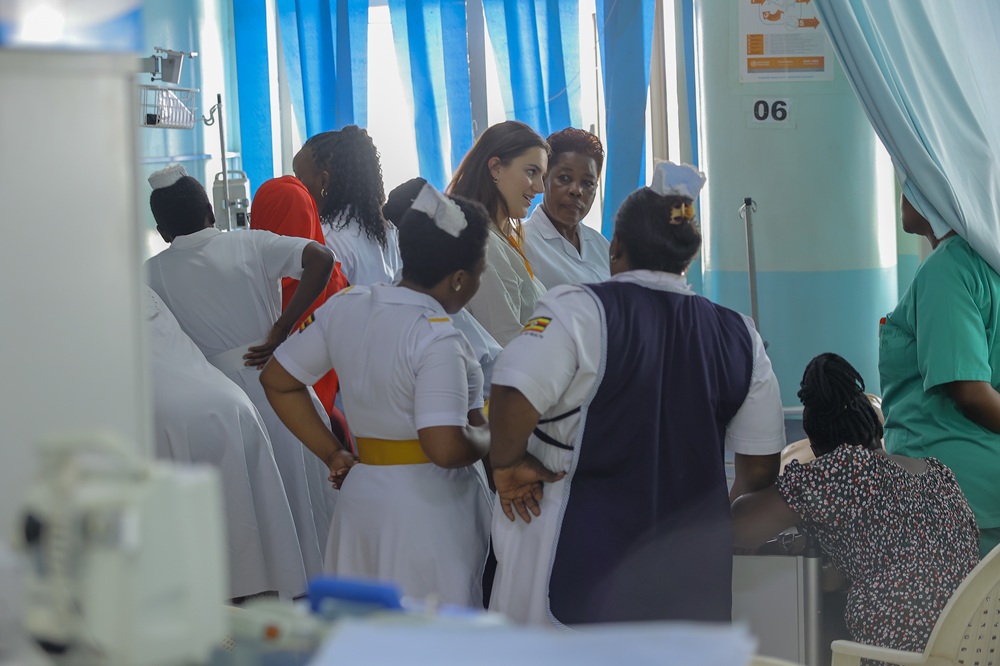
During our visit I spent time in both Mulago and Kawempe Hospitals. Some of my key tasks included delivering sessions on the assessment of acutely unwell patients, adult Basic Life Support (BLS) with the use of a defibrillator, and delirium. I did this through a mixture of simulation-based teaching and presentations. I also explored topics that the staff wanted to expand their knowledge on, such as Arterial Blood Gas (ABG) analysis.
Our BLS simulation sessions were particularly effective in reinforcing essential skills and boosting staff confidence in role allocation and structure when managing an emergency situation. We were also able to tie this into their assessment of the unwell patient (A-E assessment). This was conducted in a safe environment using the simulation mannequins which allowed them to practice working as a team and help build their critical thinking.
Many of the participants in these sessions were proactive and demonstrated amazing leadership skills. It was also a shared learning experience as they explained how they would manage a situation differently if they didn’t have the resource available. For example, using a spoon to manage an airway instead of a Guedel airway (a rigid plastic tube that sits along the top of mouth and ends at the base of the tongue). This engagement with the activity highlighted how proactive and keen they were to learn and share knowledge. I hope this inspires the local team to continue regular simulation sessions and BLS refreshers. In the long term, this exposure will enhance patient care, improve response in critical situations and contribute to a more confident team.
This was a key responsibility for us: ensuring teaching sessions were sustainable. This was made possible by the healthcare professionals in Uganda being so grateful and keen to share and learn. You could see how effective the train-the-trainer programme (run by CUH resuscitation officer Margaret Baron-Catuday) had been, because during group sessions the team would actively collaborate, sharing with us their knowledge and skills, which was amazing to see.
I believe exposure to different health systems, values, and approaches fosters more culturally competent care and encourages UK professionals to re-evaluate our services, potentially making them more inclusive, efficient, and patient-centred.
My impact
My experience of teaching compared to the rest of the team was minimal, but I was eager and enthusiastic to learn and as a result I had the most rewarding experience. I was able to observe my colleagues and present my own teaching sessions which was a great learning experience and made me keen to become a better learning facilitator in my home environment.
I had a genuine interest in the Ugandan healthcare system and definitely learned just as much as I shared. I hope that my presence helped reinforce that collaboration and mutual learning are at the heart of global health partnerships.
A highlight was the end of each teaching session, when the Ugandan nurses would sing a song to thank us for sharing our knowledge and teaching them. It was the most lovely and heart-warming way to end the day.


Challenges and rewards
The most rewarding part was traveling with a team of inspirational nurses and midwives. Working with this team of amazing people made me proud to be a nurse. The passion and dedication of the nurses and other professionals from both Mulago and Kawempe Hospitals was also astounding. The knowledge and skill set they have is so diverse to cope with the scarce resources and staffing levels, yet I never heard any complaints. I only saw resilience.
I think what really highlights how beautiful the Ugandan people are is their sense of community. They care and look after each other in a way that is so different to that of the UK and something we should aspire towards.
The challenge has been returning to the UK and seeing with a fresh perspective just how much the NHS offers people and the unfairness that the same level of healthcare isn’t available worldwide. Projects like this one are making such a difference and I hope to be able to continue to be a part of it.
Developing a passion for global health
The experience I have had has changed me as a person and as a nurse. I feel truly inspired by everyone this project has exposed me to: it has made me passionate about global health and given me some direction for where I would like my career to go. It has given me resilience for hard shifts and made me grateful for the resource we have available in the UK.
Working within the NHS and caring for patients is a privilege I’ve come to truly appreciate. I hadn’t recognised the full extent of resources and treatments options that are available to our patients or how fortunate we are to access them freely.
What made the experience even more meaningful was witnessing and becoming part of the genuine friendships formed between the Ugandan and UK colleagues over the years. These connections go far beyond professional collaboration; they’re lasting friendships that are truly special.
This project gave me the chance to travel to a part of the world, meet people and embrace a culture I may never have otherwise witnessed, and for that, I’m incredibly grateful.
Growing professionally
I have had the pleasure of working with members of the practice development team and learnt so much from them about teaching and delivery. I also worked alongside my midwifery colleagues and learnt a lot about their jobs. Working with all these people has broadened my aspirations and made me realise that I may like to be a practice development nurse in the future. The experience has also given me motivation to complete the critical care course and further my education by taking all opportunities that are presented to me.
The experience I have had has changed me as a person and as a nurse. I feel truly inspired by everyone this project has exposed me to: it has made me passionate about global health and given me some direction for where I would like my career to go.
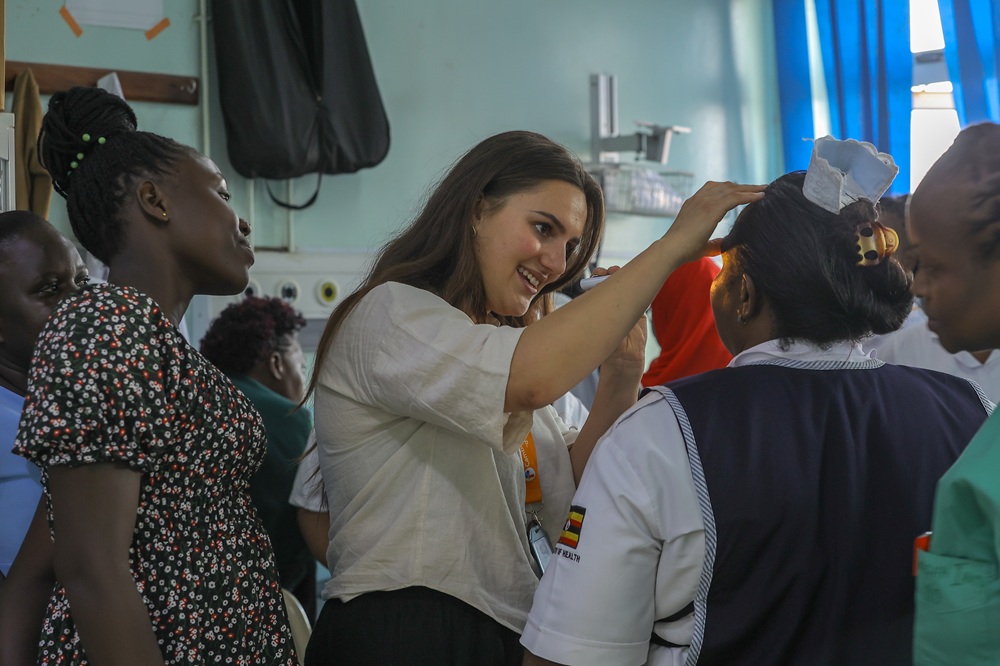
Bringing learning back into the NHS
I truly believe that teaching in Uganda not only contributes to strengthening healthcare locally but also offers us valuable lessons about how to improve practice in the UK. One of the most significant impacts is my renewed appreciation for resources and adaptability. Teaching in Uganda highlighted to me the power of peer-led learning and low-cost simulation. The use of simple materials and scenario-based teaching can easily be adapted to UK settings to improve accessibility and engagement in training, particularly in some of the under-resourced trusts.
Following on from this, I think a shift towards more value-based care is important. We should focus more on what truly is making a difference for our patients rather than relying on high-tech interventions. I also believe exposure to different health systems, values, and approaches fosters more culturally competent care and encourages UK professionals to re-evaluate our services, potentially making them more inclusive, efficient, and patient-centred.
I couldn’t recommend getting involved in global health enough. By participating, I have met and learnt from the most incredible people, from a part of the world it is unlikely I would have visited. It has broadened my view on what it means to be a nurse and given me inspiration for where I would like to progress in my career.”
Find out more about the SCALE Critical Care Project, the CGHP Grant Scheme, or contact us at info@cghp.org.uk
Return to blogs